Value-based healthcare model has transformed much of the health sector. Such a trend is expected to continue to change operations, payment structures and the way health organizations approach in delivering and evaluating services. At present, many healthcare providers are addressing the need for payment analytics to help payers operationalize contracts. For instance, few have created automated technology that enables collaborative risk sharing between healthcare suppliers and providers while there are also companies who have partnered with providers to help them understand patients in a better manner and collect payments more efficiently by using root cause analysis of denials payer contract variances. In the market, one could different models for implementing value-based care (VBC), however, the broad goal behind VBC programs is to shift the focus from quantity of procedures to a stronger emphasis on positive patient outcomes. For example, in few pay-for-performance VBC models, payers may incentivize providers to offer more preventative care services by adjusting the amount paid on traditional fee-for-service pricing if the provider reaches specific performance thresholds. A healthcare company adopting value-based model software’s can create efficiencies when implemented and executed well. For example, an organization could help better coordinate services by reducing the chances of unnecessary procedures that may be performed through such solutions. And since there is a greater focus on communication between different services offered, this model can also ensure that diagnoses and effective treatments are offered more quickly. Such factors are driving the adoption of value-based reimbursement software market.
Request for Sample Copy of This Report@ https://www.absolutemarketsinsights.com/request_sample.php?id=847
With the current COVID-19 pandemic and economic recession, there is an accelerated transition for value-based care as employers and consumers look for ways to manage spending, driving the demand for value-based reimbursement. During the first COVID-19 surge, many providers who transitioned to value-based fared better than those who leaned entirely on fee-for-service models. The transition to value-based reimbursement from fee-for-service models is anticipated to create a demand for value-based reimbursement software market in the near future.
The detailed research study provides qualitative and quantitative analysis of value-based reimbursement software market. The market has been analyzed from demand as well as supply side. The demand side analysis covers market revenue across regions and further across all the major countries. The supply side analysis covers the major market players and their regional and global presence and strategies. The geographical analysis done emphasizes on each of the major countries across North America, Europe, Asia Pacific, Middle East & Africa and Latin America.
Enquiry Before Buying @ https://www.absolutemarketsinsights.com/enquiry_before_buying.php?id=847
Key Findings of the Report:
- The value-based reimbursement software market was valued at US$ 1,516.79 Mn in 2020 and is anticipated to reach US$ 2,973.66 Mn by 2025 growing at a CAGR of 20.22% over the forecast period (2021 – 2029).
- By offerings, services accounted for the major market share in 2020 and is expected to maintain its dominance over the forecast period.
- In organization size, large enterprises accounted for the highest share in value-based reimbursement software market in 2020.
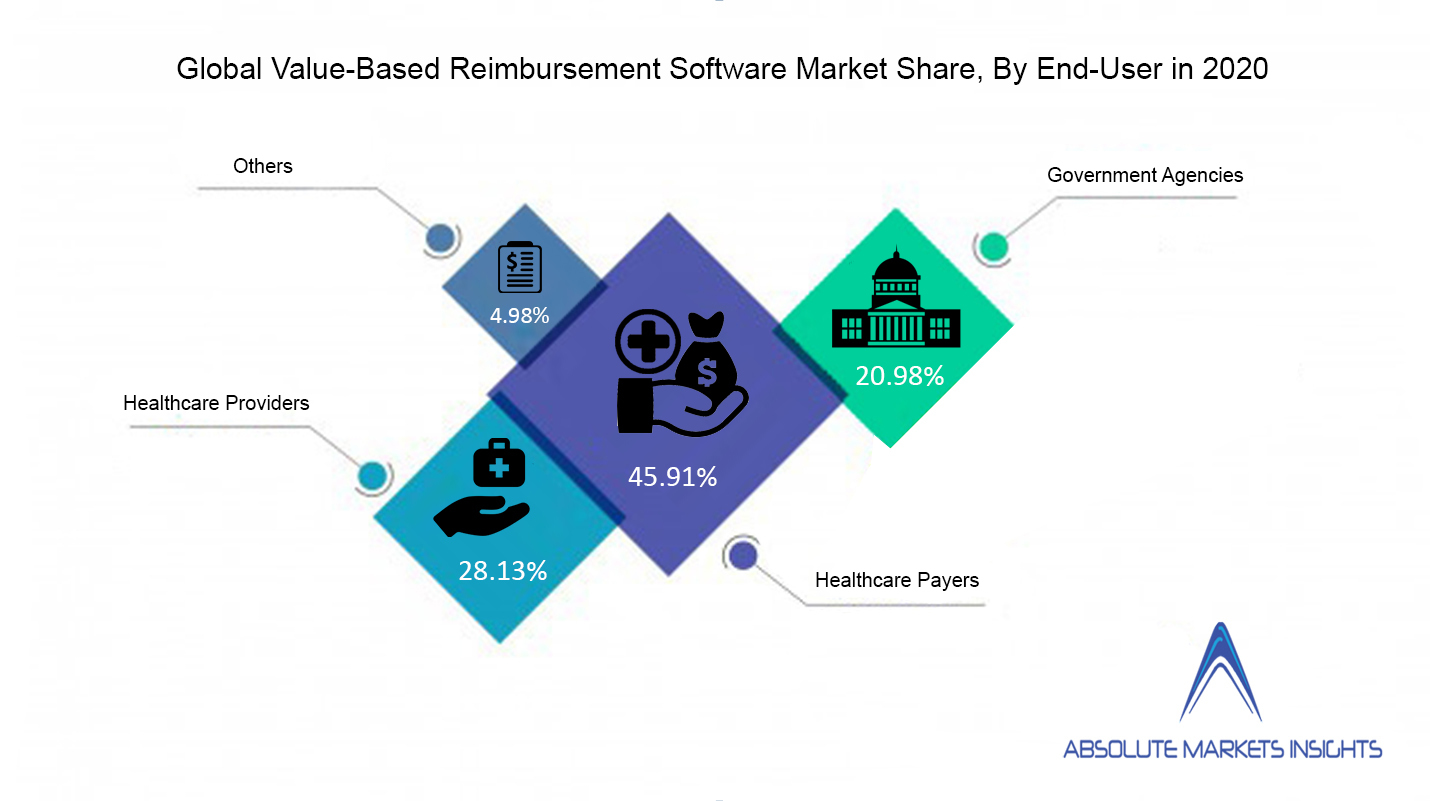
- By end-users, healthcare payers accounted the highest market share in 2020.
- By model type, Accountable Care Organizations (ACOs) accounted for the highest market share in 2020.
- By region, North America accounted for the highest share in the value-based reimbursement software market.
- Some of the players operating in the value-based reimbursement software market are 3M, Aver Inc., Change Healthcare, Cognizant, Darena Solutions LLC. (My MIPS Score), Edifecs, ForeSee Medical Inc., HealthEdge Software, Inc., LexisNexis Risk Solutions Group, naviHealth, Inc., NEXTSTEP SOLUTIONS, INC., nThrive, Inc., Quadax, Inc., RevenueXL Inc., Signify Health, VIGILANCE HEALTH, INC., Lyfegen HealthTech AG., other market participants.
Request for Customization@ https://www.absolutemarketsinsights.com/request_for_customization.php?id=847
Value-Based Reimbursement Software Market
By Offering
- Solutions
- Cloud
- On Premise
- Services
By Organization Size
- Small and Medium Enterprises
- Large Enterprises
By End-Users
- Healthcare Payers
- Healthcare Providers
- Government Agencies
- Others
By Model Type
- Pay-for-Performance
- Shared Savings
- Shared Risk
- Bundled Payment/Episode of Care
- Accountable Care Organizations (ACOs)
By Region:
- North America
- U.S.
- Canada
- Mexico
- Rest of North America
- Europe
- France
- The UK
- Spain
- Germany
- Italy
- Nordic Countries
- Denmark
- Finland
- Iceland
- Sweden
- Norway
- Benelux Union
- Belgium
- The Netherlands
- Luxembourg
- Rest of Europe
- Asia Pacific
- China
- Japan
- India
- New Zealand
- Australia
- South Korea
- Southeast Asia
- Indonesia
- Thailand
- Malaysia
- Singapore
- Rest of Southeast Asia
- Rest of Asia Pacific
- Middle East & Africa
- Saudi Arabia
- UAE
- Egypt
- Kuwait
- South Africa
- Rest of Middle East & Africa
- Latin America
- Brazil
- Argentina
- Rest of Latin America
Get Full Information of this premium report@ https://www.absolutemarketsinsights.com/reports/Value-Based-Reimbursement-Software-Market-2021---2029-847
About Us:
Absolute Markets Insights strives to be your main man in your business resolve by giving you insight into your products, market, marketing, competitors, and customers. Visit …
Contact Us:
Email id: [email protected]
Contact Name: Shreyas Tanna
Phone: +91-740-024-2424